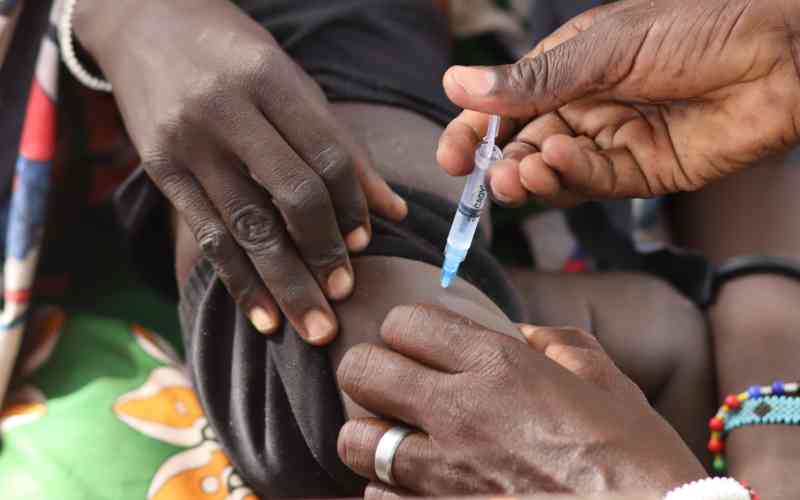
A doctor offering telemedicine services. [Courtesy]
The room is well-lit, and inside, Caroline Jebiwott holds her four-year-old daughter while a clinical officer checks his medical machines.
The medical video is attached to the computer, and the clinician signs in to the platform using the same credentials as the doctor.
After exchanging pleasantries, the clinician introduces the patient, Meghan Chepkiech, and her mother, Jebiwott, desperately trying to understand what was happening to her daughter.
Jebiwott, a health promoter in Ngoron, Tiaty Sub-county, has been vocal in promoting healthcare services and telemedicine.
This time, it was her daughter hooked on the screen, ready for examination following a two-year rash problem.
“I have seen several consultants and dermatologists, but the problem has persisted. When I heard of the roving telemedicine service, I knew it was time,” she says.
The doctor, based at Gertrude Hospital, examined her daughter after the clinical officer explained Chepkiech’s medical condition.
The clinician put her telescope on Chepkiech as the paediatrician put it in her ears as she examined her virtually, with the clinician holding the telescope to check her vitals.
With the help of a medical video for visualisation, the doctor requested to see the rash that had been disturbing Chepkiech.
Upon examination, Chepkiech was given prescriptions, which her mother said were available at the clinic.
“I believe and have faith that my daughter will be cured. I have tried seeking medication, but what amused me is how technology has been used to cure and save time,” she said.
Her daughter had an oral and skin rash.
Just like Jebiwott, Jennifer Karengei from Tirioko stares at her 12-year-old daughter Jelangat Ndege with a beam of hope flaring on her face. She smiles, expressing a tale of painful experiences she went through in search of medication.
She has seen it all. She comes from a marginalised, vast, remote village that has been neglected by previous regimes and betrayed by its own county government and leaders, and has continued to lag behind in terms of development.
Karengei faced frustration with accessing medical care for her daughter, who developed the condition over five years ago.
The Standard conducted an interview with her at Ngoron Dispensary, where she had brought her daughters, Ndege and Jepchumba Dickson, for follow-up check-ups with a roving telemedicine service.
The joyous mother held her two daughters. Despite the language barrier, one would still notice the relief as she described how her daughter was recovering well, thanks to telemedicine. The girl was diagnosed with acute kidney disease.
Her journey seeking medication for Ndege forced her to travel across counties, hoping to save her daughter from the pain.
“I have travelled across counties; my journey was a rocky one. Around 2018, my daughter developed a condition. She complained of stomach pain, she couldn’t stand, and her cries were deafening. I knew I needed to get her help as the traditional herbs had failed to halt the pain,” she said.
She took her daughter to West Pokot Hospital for medication and later to Kitale, hoping she would get the cure.
Being a member of the community, she heard of the telemedicine programme at Chemolingot Sub-county Hospital and decided to give it a shot.
“The stars were with me, finally. I saw the light. My struggle came to an end. My daughter was diagnosed and put on medication. I don’t know how the doctor diagnosed her while far away but I know she is now free from pain,” Karengei added.
To add salt to injury, her four-year-old daughter had a convulsion.
At first, the child was diagnosed with epilepsy. But the situation worsened and she took her to Chemolingot where she was diagnosed with convulsive disorder.
“I brought my daughters for a check-up, not because they were sick, but only to confirm their progress,” she told The Standard.
She says she used to travel kilometres seeking health care services and even sold her livestock for medical expenses.
Gladys Kuket, a nutritionist at Ngoron Dispensary, says her son Dennis Panga developed a headache problem for almost a year.
Each time she went to hospital her son was given painkillers, but the pain persisted.
“He would undergo excruciating pain, saying he felt blood pumping in his head. I took him to the Chemolingot Sub-county Hospital for laboratory tests but was given painkillers and told to go home,” she says.
She decided to seek a second opinion at Sigor in West Pokot County but was shocked when her son was given painkillers without a proper diagnosis.
The desperate mother later learnt from a community health promoter about telemedicine at Chemolingot and opted to seek help.
“I had nothing to lose as the medicine was not working so I tried. My son was examined by the doctor, who, I learned, was at Gertrude, Nairobi, and diagnosed with high-level haemoglobin, a condition called polycythemia,” she explained.
She was given a prescription and went home with her son after completing the medicine. Her son has never complained of the pain.
Kuket believed that telemedicine would help the locals get fast medical services and solve the high cost of transport.
“I used Sh1,500 to travel to Sigor, meaning I needed at least Sh5,000, which was quite expensive. But this telemedicine has come to save the area,” she says.
Jebiwott says she referred the two women to Chemolingot following their struggle in accessing health services and getting the right care for their children.
Telemedicine has helped in reducing referral cases among children in Tiaty since 2021, following a partnership between Safaricom Foundation, Gertrude Hospital, and the county government of Baringo.
Joseph Ouko, a monitoring and evaluation specialist at Gertrude Hospital Foundation, says Daktari Smart is a telemedicine programme that allows children to access medical care in remote areas lacking access to paediatric speciality care.
“This region is understaffed and is marginalised, specifically in accessing special care. The sub-county hospital doesn’t have a resident paediatrician, meaning that children from the area cannot get speciality paediatric care. So we are here to use telemedicine to help children access health care services,” Ouko said.
He says the situation of limited paediatricians within the country has forced the Gertrude Foundation to bridge the gap as most paediatricians were stationed in major towns.
Ouko says the gap has forced patients to travel long distances in search of paediatric care.
Telemedicine, he says, is a concept where technology is used to bring health care closer to people by bridging the gap between the patient and the doctor and ensuring that children are seen by a doctor far away from them without the need for travelling.
“We employ technology that uses video conference facilities and can provide real-time diagnosis by paediatricians in Nairobi, seeing children in far-flung areas, “he said.
The machine has medical devices connected to it, enabling the doctor to interact with the patients and would probe, investigate, and diagnose the child in real time.
The programme started in 2021 in Baringo and other counties such as Samburu, Homa Bay, Lamu, and Narok, with Baringo having two centres in Baringo South and Tiaty Sub-counties due to its vastness.
He stated that over 3,500 children from Baringo were diagnosed and referred through the health care system.
Ouko says Gertrude partnered with counties in providing service, and that after a child has been diagnosed, they are referred through existing public health structures for diagnosis and treatment.
“We provide access to a specialist who helps with early and accurate diagnosis,” he added.
First, the patient gets in contact with a clinical officer or nurse in the facility and is assessed by the medic, and the complex cases are referred to telemedicine, with a doctor waiting on the platform.
Wilson Biwott, a clinical officer and the coordinator of telemedicine in Baringo, says telemedicine is a system where paediatric patients are seen through a computer-based system, which is connected to vital organs, with the doctor able to listen and see the vital signs.
“It is a referral system where patients get to be attended by paediatricians. Due to the lack of paediatricians in Baringo, patients referred to Baringo County Hospital refuse to go due to language barriers, with others opting for traditional and alternative methods,” Biwott said.
Telemedicine, he says, has helped reduce referral cases and allowed patients to access specialists. He observes that five patients have so far had complex heart surgeries performed.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.